"Obesity represents a major health issue as it increases the risk of several diseases, including diabetes and cardiovascular disease. In addition to promoting weight loss, there is a need for the identification of novel therapies aimed at reducing the health implications of obesity. The findings described in this article will pave the way for further translational studies on the correction of a dysfunctional adipose-nervous communication in obesity.
Elisa Duregotti, Research Associate at KCL
28 November 2022
Researchers from King's identify new potential molecular mechanism in obesity
This study identifies neuronal growth regulator 1 (Negr1) as a factor that promotes neuronal growth and protects from the excessive fat accumulation characterising obesity
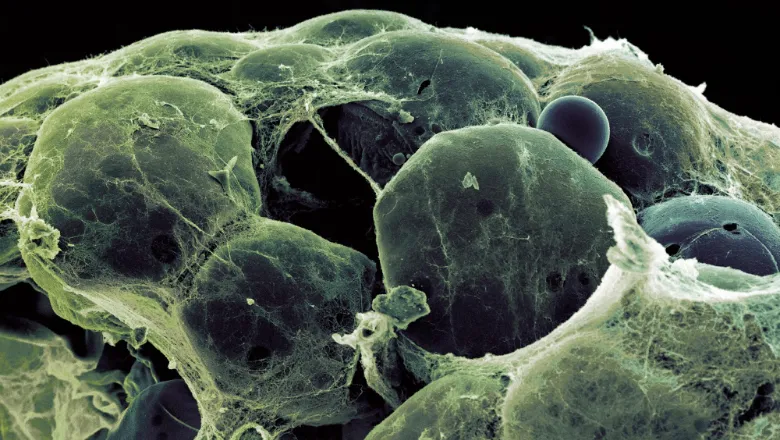
Adipose tissue is a type of connective tissue mainly composed of fat-storing cells but also including capillaries, immune cells and nerves. The neurons in the adipose tissue are controlled by the sympathetic nervous system, which promotes the burning of fat in response to certain stimuli, such as cold exposure. This process is called non-shivering thermogenesis and is known to be protective against obesity.
While certain types of fat like white and brown adipose depots have been extensively investigated, there is comparatively less research into perivascular adipose tissue (PVAT) which surrounds the vasculature. As well as storing lipids, PVAT is endowed with a secretory activity which regulates the proper functioning of the nearby blood vessels.
To better understand how obesity affects the physiology of PVAT, researchers based in the Mayr Lab used proteomic techniques to compare the secretory profile of PVAT samples with that of traditional brown and white fat depots in lean and obese mice.
A first analysis conducted on samples from lean mice revealed that PVAT secretomes are enriched for proteins involved in neuronal development. This is paralleled with a higher amount of sympathetic nerves contained in PVAT compared to other adipose depots.
In PVAT samples from obese mice, however, the number of sympathetic neurons was decreased compared to lean mice. Similar findings were obtained in epicardial fat samples collected from around the coronary arteries of obese patients.
This neuronal loss may be due to decreased secretion of neuronal growth regulator 1 (Negr1) by obese fat. Negr1 is indeed found to promote neuronal growth and to protect from neurodegeneration both in vitro and in vivo.
This is of particular interest given that some DNA mutations in close proximity to the NEGR1 gene have been identified in obese human subjects, but no hypothesis have been provided so far connecting Negr1 alterations to obesity. As the sympathetic stimulation is crucial for the activation of energy-dissipating processes in fat, the neurotrophic effect of Negr1 described here represents a promising mechanism to explain Negr1 role in obesity.
This study adds to recent evidence that a disruption of the adipose-neuronal crosstalk could represent a target for future therapeutic strategies.
“Proteomics is the large-scale analysis of proteins, the building blocks of our body. Our study is the first proteomics study of the fat tissue surrounding our blood vessels. This has led to novel insights on how obesity alters the functions of this important fat depot. Obesity is a major risk factors for diseases of the blood vessels leading to heart attacks and strokes. Further studies will investigate the implication on vascular function.
Manuel Mayr, BHF Professor of Cardiovascular Proteomics at KCL

