[It] felt like they were friends, you know, because we’d seen them for so long, they were just friends with lots of skills.
An interviewee
01 February 2023
Seeing the same midwives improves birthing experience for high-risk mothers
Seeing the same midwives throughout the perinatal period makes a substantial difference to a women’s feelings of calm and confidence during pregnancy and birth, a study has found.
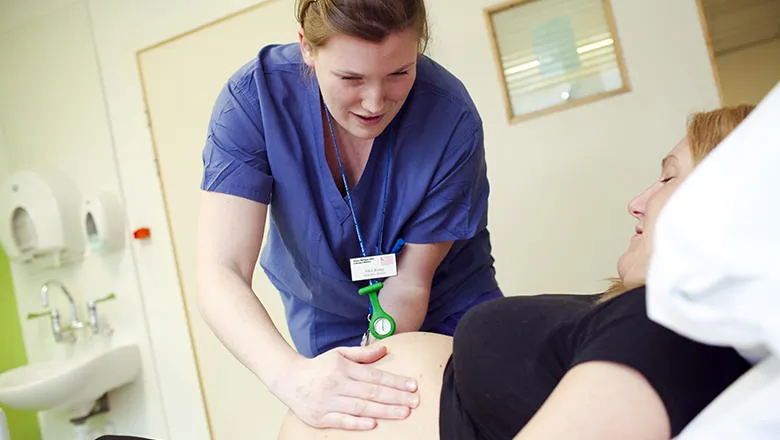
The study, published recently in Women and Birth by researchers from King’s, highlight the improvements in a woman’s experience of care under the continuity of care model.
This is the first study which looks at women’s experience of care when they are at a higher risk of pre-term birth.
The model of continuity of care is designed to provide mothers with a dedicated team of midwives who are on call 24/7 to provide support, including answering questions, provide antenatal and postanal appointments and be there for them when they go into labour.
One woman said the experience had completely changed her attitude to birth. She said: “I’m very happy that I will be able to pass on a positive message about birth to friends, my own daughter, and I don’t what it would have been like without the POPPIE team.”
The continuity of care model was set out in the NHS Long Term Plan in 2019 and the ambition is for continuity to be the default model of care for maternity services.
In reality, though, implementation of sustainable continuity models requires all building blocks to be in place such as staffing and appropriate resourcing; which can be challenging in the current NHS climate.
Interviews of women who took part in the study found they felt at ease just knowing someone was there for them all the time. Women reported never feeling rushed during appointments, and feeling like they could trust their midwife with personal information, which in turn developed trust in their midwives.
Women felt their midwives advocated for them better and navigated institutional bureaucracy for them, ensuring they were getting the best treatment.
Author Lia Brigante, a researcher from King’s College London and the Policy & Practice Advisor at the Royal College of Midwives, said: “Previous research has shown that continuity of midwifery care has a positive impact in women who are low risk or mixed risk. This paper focuses on the experience of women at higher risk of preterm birth and it shows that the model acts as a safety net, improving trust, advocacy, access and consistency of care, and reducing anxiety and stress. This study will hopefully inform policy and care provision planning for women at higher risk of preterm birth.”
Previous research has found the continuity of care model reduces the rate of preterm birth, fetal loss and neonatal death.
Lia Brigante added: “Adequate staffing and added investment is essential to ensure all women have access to the continuity model, otherwise we are in danger of implementing a two-tier system.’


