We hope this resource will help get evidence-based practices to the people that may benefit from them. While current attention is focused on the acute response to COVID, we must not forget those people already living with chronic conditions and breathlessness. This is just one way to help reduce the impact of interrupted care.
Dr Matthew Maddocks, Senior Lecturer and Specialist Physiotherapist and lead creator of the guide
07 April 2020
Helping people manage breathlessness at home
The simple guide that can help vulnerable people manage their symptoms during the pandemic.
Researchers in the Cicely Saunders Institute at King’s College London have produced a simple guide to managing breathlessness at home during the COVID-19 outbreak. The guide offers simple tips to ease breathlessness for people affected by breathlessness, their families, and those providing care. It is especially helpful for people with underlying health conditions whose clinical teams are being diverted to the COVID-19 healthcare response. The resource is harmonised with UK national guidance, including from the National Institute of Clinical Excellence (NICE) and the Association of Palliative Medicine.
What is breathlessness?
Breathlessness is the feeling of being out of breath as your lungs work harder to draw in more oxygen. It is a frightening symptom that leads to distress for patients, families and carers. Persistent breathlessness is when this continues long-term, despite treatment of the underlying condition. Feeling short of breath can also be a symptom of COVID-19 and evidence so far has shown that people with underlying health conditions are more at risk of getting seriously ill from coronavirus.
The UK government has asked everyone to stay at home as much as possible and some of the most vulnerable people with underlying health conditions have been asked to ‘socially shield’ themselves using measures designed to protect them from coming into contact with the disease by minimising all interaction with other people.
How the Managing Breathlessness Guide can help
The Managing Breathlessness guide has been created to help people who suffer from breathlessness during the COVID-19 outbreak. It is a resource that primary care professionals, such as GPs, can recommend to their patients to help implement the guidance from national bodies. Researchers and clinicians at the Cicely Saunders Institute created the guide using the best available evidence and resources, adapted for the COIVD-19 context, and with input from patients and the public.
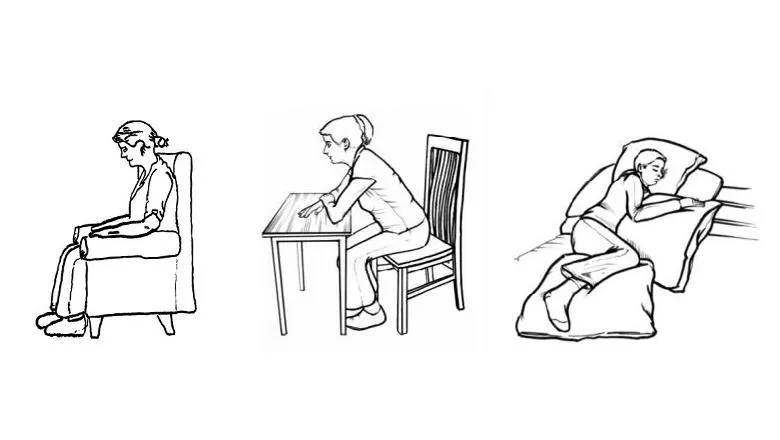
The guide offers several different steps that can help manage breathlessness and advises people to try them and use the ones they find work best for them. This includes finding comfortable positions which ease breathlessness, breathing exercises and tips to use when walking, eating and drinking or when feeling anxious. The guide also reassures people it is ok to contact their usual health and social care team for support and provides additional resources for people with breathlessness.
The resource is available to view online or download as a PDF. See links below.
