The fact that in most centres advanced imaging is not currently being implemented suggests that the development of efficient, harmonised and validated advanced MRI sequences is required to enable this.
Dr Tom Booth
18 November 2020
Nationwide imaging survey reveals varied follow-up protocols for tumour patients, prompts further investigation
There is an urgent requirement for a validated post-operative imaging protocol with definitive evidence that outcomes are improved
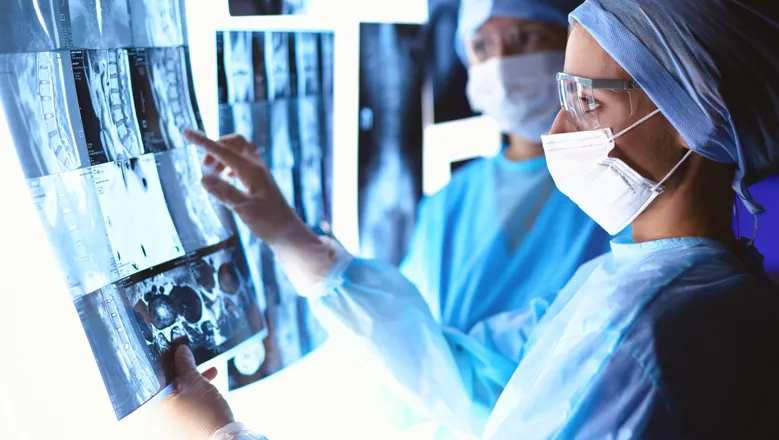
New research from The School of Biomedical Engineering & Imaging Sciences has revealed a variation in practices in the treatment and follow-up periods of glioblastoma, an aggressive cancer in the brain or spinal cord, among 31 neuro-oncological units in the United Kingdom. It is the first study to unequivocally capture UK neuro-oncology imaging practices by achieving a 100 percent response rate across three specialties from lead or joint lead consultants at all UK neuro-oncology centres.
Lead researcher, Dr Thomas Booth said the research, recently published in European Radiology, has shown there is an urgent requirement for a validated post-operative imaging protocol with definitive evidence that outcomes are improved.
“In our study we have now quantified the heterogeneity across the UK and the results unequivocally demonstrate the variation in imaging practices in the treatment and follow-up periods of malignant brain tumours,” Dr Booth said.
“In particular, during adjuvant chemotherapy treatment -- chemotherapy along with other treatments – there was considerable variation in the timing and frequency of imaging.”
The survey also required participants to state what ideal imaging practice would look like.
Neuroimaging experts tended to want to increase the amount of advanced imaging at each imaging session, essentially an MRI toolbox to allow the assessment of physiological biomarkers of tumour growth.
Dr Booth said the baseline data from this study shows evidence-based change for scanning protocols is required nationally.
“Achieving evidence-based rationalisation and harmonisation of imaging is the next step,” he said.
He said the subsequent benefits may lead to a reduction in ‘scanxiety’, anxiety associated with the process of cancer imaging and the results obtained, and plausibly clinical outcomes.
To achieve optimal practice in this heterogeneous patient pathway where there are multiple co-variates, large, multicentre, longitudinal, prospective trials that are possibly informed by data-driven machine learning algorithms are required.
Doing this is challenging because whilst devastating - causing more adult working years of life lost than any other cancer - malignant brain tumours are not very common. here are several molecular signatures and there are lots of potential management decisions along the pathway.
“A large amount of data is required in order to include all these combinations yet tease out the influence of imaging, large and therefore by default multicentre,” Dr Booth said.
“To ensure the evidence obtained is of the highest quality, the studies should also be prospective.”
“There is also an opportunity for modelling and machine learning algorithms to contribute here.”
Some work has already commenced at The School of Biomedical Engineering & Imaging Sciences at King’s College London, where Dr Booth’s team is exploring evidence-based imaging of malignant brain tumours and are aiming to provide solutions.
Dr Booth said future work is with the involvement of collaborators from the National Cancer Research Institute (NCRI) network and includes UK brain tumour charities.
“Dr Aysha Luis, Neuroradiology Fellow and also Co-Lead of the paper, is exploring an alternative method for imaging patients with malignant brain tumours,” he said.
“Alysha Chelliah a PhD student from the School is modelling the malignant brain tumour pathway and applying machine learning techniques.”
To overcome common problems in malignant brain tumour imaging where the results are non-specific, Haris Shuaib, Medical Physicist and PhD student, is using machine learning.
There are also prospective multicentre studies aimed at analyses of malignant brain tumour imaging data.

